Share this
What Is Infection Control & Where Is It Most Important?
by HEPACART on Apr 15, 2020
With the COVID-19 pandemic at hand, infection control is more critical than ever.
As this is being written in the spring of 2020, the question of how far coronavirus disease 2019, COVID-19 for short, will spread is still unknown. However, its effect on society and the economy is already reaching historic proportions.
As public health officials ramp up mitigation, sports events and public gatherings are being canceled. Colleges are telling students not to come back after spring break, but to work online. Washington state has banned public gatherings of more than 250 in three counties in the Seattle area. The first containment zone has been set up in New Rochelle, New York, Disney is closing its theme parks, and Congress is meeting over an emergency aid bill for hourly-wage Americans who live paycheck to paycheck. The stock market has lost a third of its value, with no bottom in sight, which will have long-term devastating effects on the world financial system.
With the coronavirus now officially a pandemic and spreading exponentially, it is hard to know where things will stand as you read this a couple of weeks after the World Health Organization's March 11 announcement.
While epidemiologists are getting a workout as world leaders look to them for guidance about COVID-19, professionals such as infection control directors, infection preventionists, nurses, and healthcare facility managers are preparing for the possibility of an overwhelming influx of patients, triggering shortages of critical medical resources and supplies.
Against this backdrop, a blog post about infection control may seem more than ordinarily relevant. However, the fact that 1 out of 25 (or 30 as estimates vary) hospital patients have a healthcare-associated infection (HAI) certainly merits attention on its own.
Where is infection control important?
According to the Office of Disease Prevention and Health Promotion (ODPCP)'s recently-published page on HAIs, here are some of the care settings where HAIs are an issue:
- Acute care hospitals
- Ambulatory surgical centers
- Dialysis facilities
- Outpatient care (e.g., physicians' offices and health care clinics)
- Long-term care facilities (e.g., nursing homes and rehabilitation facilities)
Obviously, concern over HAIs is not just for hospitals, but for any environment where healthcare is provided.
What exactly is infection prevention and control?
Infection prevention and control is defined as a practical sub-discipline of epidemiology, focused on preventing HAIs.
Since we're doing an overview of the topic's importance to hospitals, nursing homes, and other healthcare environments, let's ask two basic questions:
- What are the most common sources of HAIs?
- What are the top practical measures to prevent HAIs?
ODPCP says common HAIs include the following:
1. Catheter-associated urinary tract infections
2. Surgical site infections
3. Bloodstream infections
4. Pneumonia
5. Clostridium difficile
While the list above covers infections transmitted through invasive procedures, instruments, and equipment (surgery, catheters, ventilators), it omits an important category, and that is infections transmitted by air or water in the healthcare environment. An estimated 5-7% of HAIs are directly caused by construction, ranging from microbial biofilms in water pipes that are dislodged by vibration, to pathogens riding piggyback on airborne dust particles set free merely from disturbing ceiling tiles.
As discussed in our November 2019 post, Tools for Infection Control in Hospital Maintenance and Construction, a well-known pathogen that thrives in water is legionella. There are roughly 20 outbreaks of Legionnaires' disease a year affecting over 5,000 people, and 25% affected in healthcare facilities die.
Airborne pathogens can be mold spores, viruses, or other microbes, and pose a particular danger to immunocompromised patients. Once a construction project is completed, a proper deep-cleaning is essential to prevent tactile contamination from dust and bacteria on surfaces.
Implement these critical infection prevention measures.
Here are a few of the top practical measures for preventing the person-to-person spread of infection.
Prevention measure #1: Hand hygiene

According to the U.S. National Library of Medicine, proper hand washing is the most effective way to prevent the spread of infection in hospitals. To improve the rate of hospital staff handwashing compliance (an abysmal 48% among nurses, 32% among doctors in this 2010 study), we suggested the following practical measures in our September 2019 post 6 Infection Control Strategies for Healthcare Facilities:
- Additional strategically-placed signage
- Increased staff education
- More hand sanitizer stations at key locations
- Continuous electronic monitoring of handwashing
It's critical to note that rubber gloves should be used only after thorough handwashing, not as a substitute for it. Detailed information on hand hygiene can be found on this CDC summary of recommendations under IV.A. Hand Hygiene.
Prevention measure #2: Respiratory hygiene

Preventing transmission from one person to another via droplets propelled by a sneeze, or by contact with respiratory secretions, comes down to education, a well-equipped environment, and proper use of personal protective equipment (PPE - see #3). Signs should be posted instructing patients and others with symptoms of respiratory illness to cover their noses and mouths when sneezing or coughing, use and dispose of tissues, and wash hands afterward. Sinks, dispensers of alcohol-based hand rubs, and foot-operated receptacles for waste should be strategically placed in both ambulatory and inpatient settings.
Prevention measure #3: Use of personal protective equipment
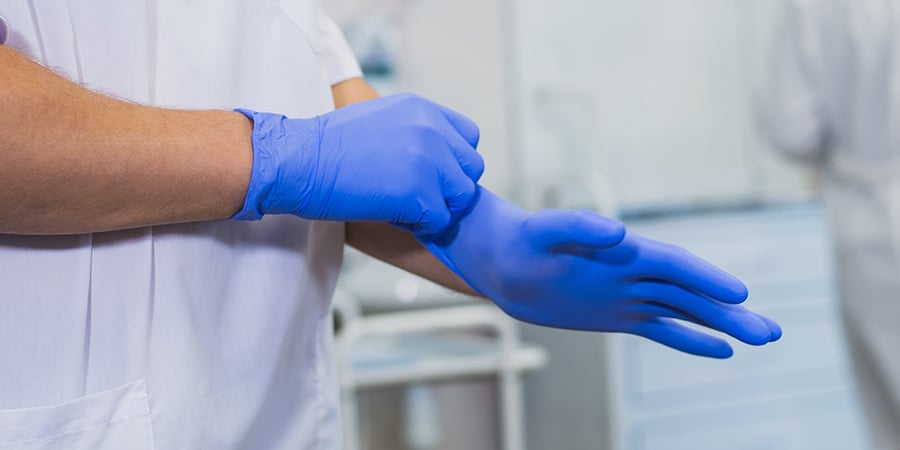
Medical personnel who come into contact with infected patients must use personal protective equipment that creates a barrier between the worker and the infectious material. Depending on the severity of the risk, PPE ranges from simple to complex. According to CDC's Guidance for the Selection and Use of PPE:
- Disposable gloves protect hands
- Gowns, aprons protect skin, clothing
- Masks, respirators protect mouth, nose, respiratory tract
- Goggles, face shields protect face, mouth, nose, and eyes
Just as important as using PPE is following proper protocol when using PPE, such as observing the basic principle of "working from clean to dirty," avoiding such faux pas as touching environmental surfaces such as light switches and cabinet knobs with contaminated gloves.
Conclusion
While it's beyond the scope of this article to address solutions to common HAIs such as surgical site infections or urinary tract infections from catheters, these topics and their solutions are well known in the medical community. An excellent overview of the subject is contained in Chapter 41 of Patient Safety and Quality: An Evidence-Based Handbook for Nurses and Chapter 41: Preventing Health Care-Associated Infections.
For a brief overview of preventing construction-based HAIs from airborne dust, download our Tools for Infection Control White Paper.
Resources
|
Infection control blog posts |
These are our blog posts tagged with the keyword "infection control" |
|
Centers for Disease Control (CDC) has vast amounts of information on infection control |
|
|
Infection Control |
A wealth of information and links to resources |
|
Infection Control Responsibilities in Senior Care and Nursing Homes |
Blog post pertaining to infection control as it relates to senior care and nursing homes |
|
Interview with the Director of Infection Prevention and Control |
Blog post from director of infection prevention and control at Sunnybrook Health Sciences Centre in Toronto |
|
Simple overview of how infections spread in healthcare settings |
|
|
Standard and transmission-based precautions, with links to posters and further information |
|
|
Valuable CDC guidelines specifically concerning environmental infection control. |
|
|
Guidelines for Environmental Infection Control in Health-Care Facilities |
Valuable CDC guidelines specifically concerning environmental infection control. |
|
CDC guidance on other aspects of infection control |
|
|
Useful page with links to 19 PDF checklists to assess infection prevention for hospitals and ambulatory care facilities. |
|
|
All 19 CDC Infection Control Quick Observation Tool (QOT) checklists |
All CDC QUOT checklists in one PDF document |
|
Excellent summary of recommendations for preventing transmission of infectious agents in healthcare settings |
|
|
The World Health Organization's infection prevention and control pages |
|
|
Infection Control For Facilities Managers: The Complete Guide |
A go-to reference for facility managers |
|
6 Infection Control Strategies for Healthcare Facilities |
A recent HEPACART blog post with practical strategies for infection control
|
|
Healthcare-Associated Infections (ODPHP) recommendations for preventing, reducing, and eliminating healthcare-associated infections |
|
|
Guidance for the Selection and Use of Personal Protective Equipment (PPE) in Healthcare Settings |
This PDF provides information to improve personnel safety in the healthcare environment through appropriate use of PPE |
|
National Action Plan to Prevent Health Care-Associated Infections: Road Map to Elimination |
The ODPHP’s National HAI Action Plan |

