Share this
Tools for Infection Control in Hospital Maintenance & Construction
by HEPACART on Nov 18, 2019
Updated on August 13, 2020.
Juggling competing priorities like budget, deadlines, and infection control in an active facility is no easy task.
It's been estimated that 75% of health care construction projects consist of upgrading or expanding facilities that must continue to serve patients. For construction managers and infection preventionists, doing construction inside a working facility can feel a bit like being a mechanic trying to overhaul a transmission while running beside the customer's car.
Juggling competing priorities like budget, deadlines, and infection control in an active facility is no easy task. Every job is different, requiring deployment of a multidisciplinary team to develop a customized infection control risk assessment (ICRA).
Vibration from construction can shake loose pathogen-laden dust particles that fly through the air, and it can dislodge microbial biofilms within pipes allowing organisms to spread to faucets and showers where they come into contact with patients.
.webp?width=900&height=450&name=WhatYouNeedToKnowAboutNegativeAirMachines%20(1).webp)
Since roughly 100,000 people die each year from healthcare-associated infections (HAIs), with an estimated 5-7% of HAIs caused by construction, it's critical that your ICRA team and everyone implementing infection control precautions have the best information and tools at their disposal.
.webp?width=900&height=395&name=Content_1OutOf25HospitalPatientsHaveHAIs%20(1).webp)
In this post, we'll review some of the tools and procedures to keep both water and air pathogen-free.
Reducing Waterborne HAIs
HAIs that are epidemiologically linked to potable water, or wHAIs, can be many things, including surgical site infections, eye infections, urinary tract infections, pneumonia, even Legionnaires' disease. The ways in which water can cause HAIs are multitudinous, making dealing with airborne HAIs seem simple by comparison.
One problem is, water that's safe for drinking is far from sterile, and the biofilms that often colonize the pipes of hospital plumbing systems are complex ecosystems. Among the billions of harmless bacteria in potable water that enters from the outside, a small percentage are opportunistic pathogens such as the deadly legionella pneumophila, and they feel right at home in the friendly neighborhood biofilm.
Undisturbed, the biofilm can thrive like some microscopic Sim City without causing problems to the outside world. Then one day, vibration from construction, sudden water flow through a normally stagnant part of the system — perhaps from high demand — can dislodge microorganisms from the biofilm into the bulk water flow, and now you have bacteria, fungi and amoeba pouring out of shower heads and faucets.
One of the better-known pathogens that thrives around water is legionella. The Centers for Disease Control and Prevention (CDC) estimates that there are more than 20 outbreaks of Legionnaires disease each year, affecting over 5,000 people, and 25% of those affected in a healthcare facility die.
To reduce the risk of wHAIs, you need a water management program. One invaluable resource for anyone responsible for centralized building water systems is the 2018 edition of Legionellosis: Risk Management for Building Water Systems, which is the American National Standards Institute/American Society of Heating, Refrigerating and Air-Conditioning Engineers (ANSI/ASHRAE) Standard 188 for model programs.
Ways to reduce risk of wHAIs include using sterile water in high-risk patient areas, supplemental disinfection (either chemically, with chlorine, or by UV light sterilization), and point-of-use water filters, which have been shown to be beneficial in multiple studies, according to a 2018 Infection Control Today article, Healthcare Plumbing Systems Are Sources and Vectors of Infection for HAIs.
Reducing Airborne HAIs
Another contributor to HAIs in the healthcare environment is dust that leaps into the air every time somebody yanks a crowbar, fires a nail gun, or removes a ceiling tile. Dust thus generated is nasty stuff. See What Exactly Makes Up Dust? if you need a refresher on the grungier members of the dust community.
The most stringent dust control precautions, reserved for major projects in the vicinity of higher-risk patients, are designated Class IV by the ICRA Matrix, the guiding document for precautions to take against airborne dust during hospital construction and renovation.
ICRA MATRIX
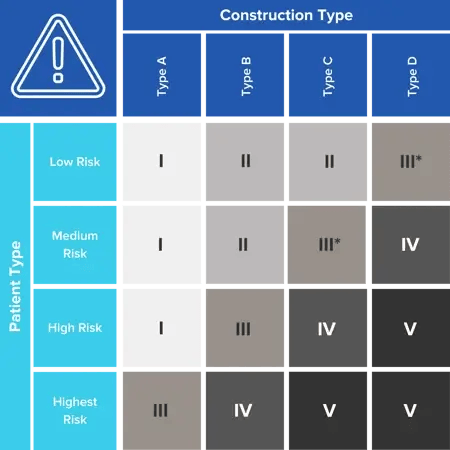
Class IV precautions include isolating the HVAC system, sealing all holes and gaps, maintaining negative air pressure to keep air flowing into the worksite, keeping workers from transporting dust out, and sampling air regularly. A slight vacuum must be maintained by constantly removing air from the room at a specified rate (typically 6 or 12 ACH, air changes per hour); air thus exhausted must be cleaned of dust and pathogens with the best mechanical filtration available. HEPA filters, which are designed to remove 99.97% of particles of 0.3 µm (micrometers) or larger from the air, are used in dust containment carts, anterooms, and exhaust panels of temporary walls used to enclose construction projects.
Common dust particles, most mold spores, and many bacteria are larger than 0.3 µm, but other pathogens such as the microbes that spread influenza and tuberculosis, or the very common aspergillus fungal spore, can slip right through HEPA filters — even those with antimicrobial coatings. In situations where there is extremely high risk from airborne-mediated disease, germicidal UV light can be integrated into air-treatment equipment.

Here are some specific examples of tools to fight airborne infection:
- Dust containment cart with integrated HEPA filtration — HEPACART®
- Negative air machine with HEPA filtration and antimicrobial pre-filters -— HEPAFORCE
- Reusable temporary airtight walls — STARC Systems RealWall and STARC Systems LiteBarrier
- Portable air scrubber for in-room air disinfection via far-UV light — Germbuster 5000
Conclusion
Many procedures and products have been introduced to eliminate HAI health hazards. Each has its merits and shortcomings. The job of the infection control solution must be to contain all contaminants and make sure they are not introduced or reintroduced into the air.
For further reading, we recommend that you download our white paper on the subject of tools for infection control.
Here are some additional resources:
- Infection Prevention Manual for Construction & Renovation
- Air Changes per Hour, Infection Control and Dust Containment
- 3 Infection Control Solutions for Class IV Construction Projects
- Why Does Construction Lead to Infection Control Problems?
- Infection Prevention during Demolition, Construction, and Renovation
- 10 Hospital Objects that Breed Infection-Causing Bacteria
- 6 Ways to Reduce HAIs

